Temporal Bone Malignancy
- Dr. Niveditha Damodharan

- Jan 18, 2023
- 6 min read
Updated: Jul 7, 2023
Temporal bone malignancies are rare tumours accounting for less than 1 percent of all head and neck malignancies. Sun exposure is associated with cutaneous malignancies and radiation exposure with Squamous Cell carcinoma. Chronic Otitis media has also been linked to temporal bone malignancy by some researchers. The most common malignancy seen is Squamous Cell carcinoma and other malignancies have been sparsely reported. Because of the rarity of these tumours, temporal bone is more likely to be involved in secondary malignancies arising from Parotid region or Periauricular skin cancers.
Origin and Spread
Most temporal bone neoplasms are epithelial neoplasms arising from the middle and inner ear including Squamous Cell Carcinoma, Endolymphatic sac tumor and Adenoid cystic carcinoma. Secondary tumours include those arising from Parotid gland, Nasopharynx, Brain and Periauricular Skin cancers. Temporal bone malignancies can arise from any part of the temporal bone including the External auditory canal, middle ear, mastoid, endolymphatic sac, petrous apex and the internal auditory canal. They can be locally aggressive due to the presence of numerous bony pathways in the temporal bone along which the tumor can spread from the site of origin.
Symptomatology
Ear discharge, Hearing loss and Ear ache form the classical triad of symptoms of Temporal bone malignancies. Long standing ear discharge, particularly resistant to conservative treatment should arise the suspicion of malignancy. Discharge can be purulent or bloody. Hearing loss can be purely conductive if the disease is confined to middle ear and ear canal. Sensorineural hearing loss occurs due to inner ear involvement. Tinnitus, vertigo and imbalance can also occur in such cases. Headache signals extension of the tumour intracranially. Trismus (Anterior involvement into Temporomandibular joint), Facial weakness, Involvement of other cranial nerves, Neck node metastasis will mean that the disease is advanced. Adenoid cystic carcinoma can present as masses beneath the skin of the external auditory canal.

Diagnostic Imaging
High Resolution Computed Tomography and Magnetic Resonance Imaging with contrast are required to evaluate the extent of the tumour. CT imaging is the best to demarcate bone involvement. MRI is superior to CT scan to delineate soft tissue involvement, perineural spread, involvement of Sigmoid sinus, Internal Carotid Artery and intracranial extension. Usually anterior and inferior spread of tumour are accurately assessed radiologically, compared to superior, medial and posterior extensions1.
Staging
No proper TNM staging system has been approved by the American Joint Committee on Cancer for temporal bone malignancy. Modified Pittsburgh system was initially proposed for Squamous Cell Carcinoma of the external auditory canal and doesn’t take into account the other subsites of the temporal bone. It also doesn’t include non-squamous malignancies. However it is the most commonly used staging system. Early-stage T1 tumors are limited to the ear canal without any bony erosion or soft tissue involvement. T2 tumors have limited bony ear canal erosion or limited soft tissue involvement. T3 tumors erode the bony ear canal or have limited soft tissue involvement or begin to involve the middle ear or mastoid. T4 are large tumors that involve the inner ear, the carotid canal, the jugular foramen, and the dura or have evidence of facial paresis. Neck nodal metastasis immediately progresses the tumour stage to stage IV.
Management
Surgery remains the standard of care for Temporal bone malignancies. Adjuvant Radiotherapy has been advised for T2 and larger tumours. Positive margins, extracapsular invasion, nodal metastasis, bony or perineural invasion are other indications for adjuvant therapy. Chemotherapy has also become an emerging adjuvant option for advanced malignancies2.
Surgical management can range from Sleeve Resection to Lateral temporal bone resection (LTBR) to Subtemporal bone resection (STBR) to Total temporal bone resection (TTBR). We do not recommend Sleeve Resection as it is difficult to achieve adequate margin. Lateral Temporal bone resection is the procedure of choice for T1 and T2 tumours with or without Superficial Parotidectomy. Both LTBRs and STBRs are accepted modalities of treatment for T3 lesions. Although TTBRs are proposed as the best modality by other centres, we prefer to do an STBR with a combination of en-bloc and piecemeal resections followed by Adjuvant Radiotherapy. Due to the increased morbidity and no proven survival benefit, we do not recommend TTBR over STBR in T4 tumours.
1. Lateral Temporal Bone Resection
This procedure involves resection of temporal bone lateral to Facial nerve and is the real workhorse of Otologic Oncologic surgeries. The procedure starts with a canal wall up mastoidectomy with extended Facial recess opening. The EAC is resected en bloc along with the tympanic membrane, the malleus after disarticulation and removal of the incus, with the medial limit defined at the level of the incudostapedial joint. Superficial parotidectomy can be done with lateral temporal bone resection (LTBR), specially in T2 tumours.
2. Subtemporal Bone Resection
This procedure is an extension of LTBR and proceeds with piecemeal removal of the tumour after the initial steps of LTBR are performed. It involves IAC identification, facial nerve exposure and removal of the otic capsule with preservation of the petrous apex. Capsule of Temporomandibular joint and condyle of mandible are removed in case of anterior extension. Dural extension may warrant middle and posterior fossa craniotomies. Facial nerve is re-routed unless otherwise involved by tumour and need to be sacrificed. Sigmoid sinus and Jugular bulb can be preserved unless infiltrated. In case of doubtful tumour clearance, a vascular clip can be left behind so that postoperative radiotherapy can be targeted at that site.

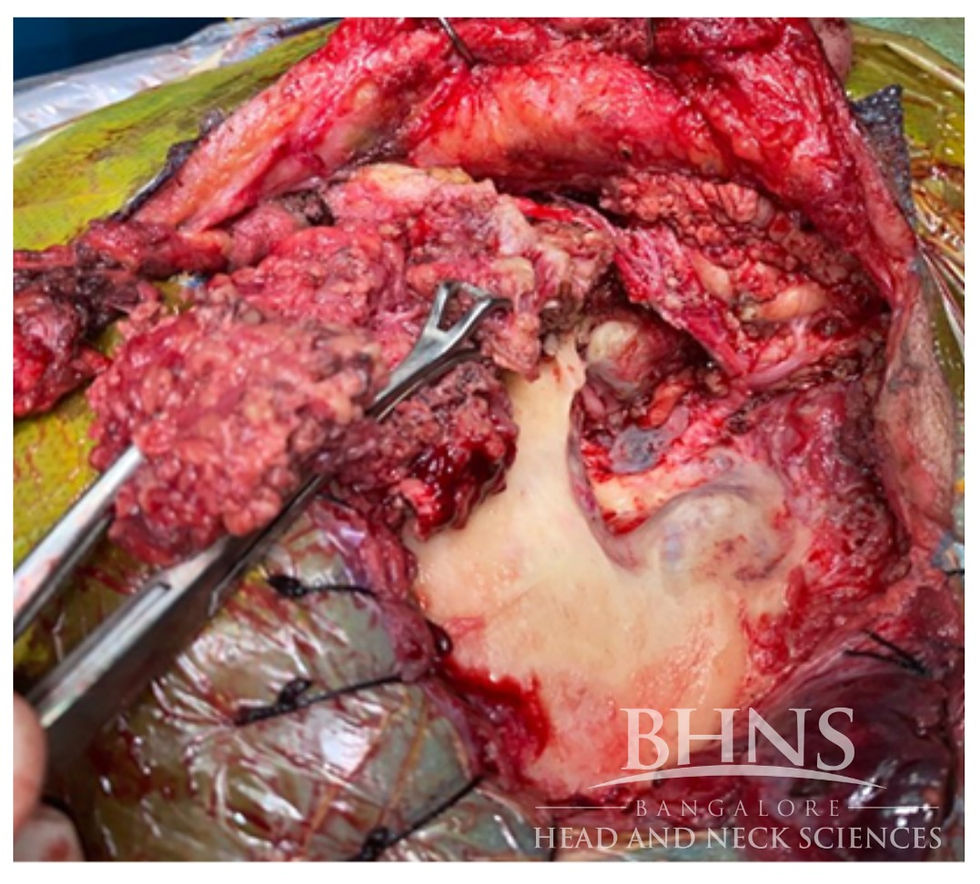
3. Total Temporal Bone Resection
This procedure is done in advanced T4 tumours. Pinna may or may not be resected. Bone is resected superiorly for 3 cm above the temporal line to expose the middle fossa dura and behind the sigmoid sinus by a similar amount to leave a residual margin of healthy bone. Medial dissection extends through the labyrinth and exposes the intrapetrous carotid artery. Inferiorly, the sigmoid sinus and jugular bulb are mobilized from surrounding bone. The sternocleidomastoid and digastric muscles are freed from the mastoid tip. The ascending ramus of the mandible is transected and removed along with the head and coronoid process. A total parotidectomy is done and the specimen is removed en bloc. The residual tip of the petrous bone is then removed with a high-speed drill. Resection of the carotid artery can also be accomplished if the contralateral cerebral blood supply has been proven to be adequate by angiography and preoperative balloon occlusion. Overall this procedure is highly morbid and has no proven survival benefit over STBR.
Piecemeal resection is preferred over en bloc resection in large tumours to minimize morbidity and preserve vital structures3. Bone is drilled until healthy bone appears.
Role of Parotidectomy and Neck Dissection
Parotid region can be involved by either direct extension through Foramen of Huschke and Fissures of Santorini or nodal dissemination to the intra-parotid or peri-parotid lymph nodes. We do not routinely perform Superficial Parotidectomy for all T2 tumours and prefer to do it in T2 tumours with involvement of anterior wall of EAC. In T3 tumours, we routinely include Superficial Parotidectomy. In T4 tumours, a total Parotidectomy is performed.
Lymphatic drainage of EAC and middle ear goes to intra-parotid and peri-parotid, pre and postauricular, submandibular, upper deep cervical and the retropharyngeal lymph nodes. Nodal metastasis has a poor prognosis. We recommend a routine neck dissection of parotid and level 2 nodes for clinically positive nodes. For N0 necks, a frozen section of level 2 nodes can be done and can proceed to neck dissection if positive for metastasis.
Hearing Rehabilitation
Maximal conductive hearing loss occurs with LTBR and can be rehabilitated with Bone anchored hearing implants (BAHA / OSIA). Single sided deafness from STBR and TTBR can be rehabilitated with Bone anchored hearing implants or CROS hearing aids Contralateral routing of signals).
Conclusion
With the advancement in neuroimaging, neuroanesthesia and skull base surgery, temporal bone malignancies can be treated surgically with minimum morbidity. However definite protocols can be formed only after proper staging systems are put into place. Further research into the different histological varieties is also required.
Bibliography
1. Leonetti JP, Smith PG, Kletzker GR, Izquierdo R. Invasion patterns of advanced temporal bone malignancies. Am J Otol 1996; 17:438–442.
2. Gidley PW, DeMonte F. Temporal bone malignancies. Neurosurgery Clinics. 2013 Jan 1;24(1):97-110.
3. Prasad SC, D’Orazio F, Medina M, Bacciu A, Sanna M. State of the art in temporal bone malignancies. Current Opinion in Otolaryngology & Head and Neck Surgery. 2014 Apr 1;22(2):154-65.












Comments